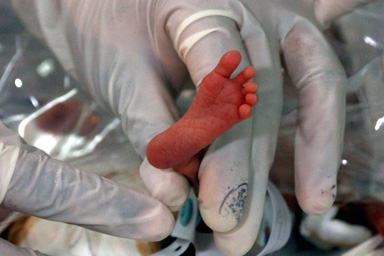
After years of trying to conceive, writer Vicki Forman’s twins were finally coming. Way too early.
Evan and Ellie were only 23 weeks gestation when Forman went into labor. They were so premature Forman thought she was having a miscarriage. At birth, each baby weighed only about a pound.
“One of life’s great illusions is the notion that we can want — and get — things on our own terms, no matter what. It’s human nature to seek pleasure and avoid suffering, but what happens when suffering finds you?” Forman writes in her harrowing new book “This Lovely Life: A Memoir of Premature Motherhood.” “My husband and I had tried for two long years to conceive these twins, had lived through miscarriages and fertility treatments to bear them. When I learned they were coming so early and so fragile, I had only one wish: to let them go.”
While Forman thought the twins should be allowed to die, their doctors struggled to save them. While Ellie lived for only four days, Evan, who endured severe disabilities including the inability to speak or see, died just shy of his eighth birthday.
“This Lovely Life” is Forman’s bracing account of becoming the mother of two super-preemies. Its drama comes not only from the relentless medical challenges that tiny Ellie and Evan faced, but also from Forman’s often conflicted emotions, as she cares for her son through his first tenuous years, navigating myriad medical crises, and becomes his greatest advocate. Yet, she feels angry and frustrated that her daughter and son were not to be among those celebrated “miracle babies” who are born terribly premature, but turn out just fine. Along the way, the book raises difficult questions about the ethics of the infertility business, as well as the rights of the parents of extremely premature children vs. the responsibilities of hospitals that treat them.
I spoke with Forman, 47, who teaches writing at the University of Southern California, by phone from her home, where she lives with her husband, Cliff, and 12-year-old daughter, Josie.
What does being born at 23 weeks gestation mean physically?
The brain is still very immature. The retinas have not developed. The lungs are not fully developed. For the most part, the rest of the fetus is fully developed, but cannot survive primarily because of the lung development. Until the advent of surfactant in the early ’90s, which is used to lubricate the lungs, babies born this early did not survive because their lungs could not provide respiration to the body.
When a baby with immature lungs respires, the lungs stick together. They can inhale, but they can’t exhale. Surfactant essentially greases the lining of the lungs so that there is more plasticity so that they don’t stick together on the inhalation.
Even a decade earlier, there is no chance that the twins would have survived?
No chance.
What was your initial reaction when the twins were born so early?
I thought I was having a miscarriage. I had had absolutely no signs that I detected as being of pre-term labor.
I was an educated person. I thought I had been trained to see the signs and symptoms, and I really knew nothing. The doctors examined me to discover that I was 7 centimeters dilated, which is effectively too far gone to stop the labor.
I was shocked and completely overwhelmed. My husband and my then 3-year-old daughter had come with me. They were there with me in the hospital in the examining room.
I knew that if the babies were to be delivered they would certainly not be able to survive. I had been informed during my pregnancy that 24 weeks was the edge of viability, so to my mind, since we had not yet reached 24 weeks, these babies would not be viable.
I felt that it was important not to intervene [to resuscitate the babies after birth], in that it would be a painful experience for them, and for me and for us as a family. It certainly felt to me that the risks of morbidity and mortality were so high that I didn’t understand why the plan was to intervene.
Why was the hospital policy in conflict with your wishes as the twins’ mother?
What I’ve come to learn is that policies regarding care in cases of extreme prematurity vary from hospital to hospital, and even, from what I’ve been able to determine, from shift to shift.
It can often be the decision of the obstetrician, or the neonatologist on duty, as to what to do in these cases. I have heard from other parents at other hospitals where they had twins born at this gestation, who were actually told that they shouldn’t resuscitate the twins. This indicates to me that there is very little consistency across hospitals at this gestation whether or not to provide care or to withhold it.
You were being told that the twins had to be resuscitated?
I was being told that I had no choice. I was told that the laws of the state of California required resuscitation because the babies would be born with signs of life. I was allowed to labor. I delivered the twins. They were both resuscitated. They were taken to the NICU [neonatal intensive care unit].
They were provided with intensive care, which included artificial ventilation and an enormous amount of drugs which are necessary to keep an infant born this early alive. Within a few days, my daughter had suffered a brain hemorrhage, and the hemorrhage was so severe that — as the doctors put it — the quality of her future life was deemed nil. They then met as a team, and allowed us to remove her from life support, which we did when she was 4 days old.
What were some of your feelings during this time?
I was deathly afraid. I had two very, very sick infants, and I had a 3-year-old who needed me at home. I firmly believed during the delivery that the twins shouldn’t be resuscitated. However, once they were born they were my children, and I began to understand that it was my job to take care of them, and to look out for them, and that if I didn’t love them, who would?
Initially, friends and even some doctors would try to arm you with stories of children who had been born this early, and turned out fine. What was that like for you?
It gave me a kind of hope, and I certainly wanted to believe the stories that they were telling me. I remember commenting to a friend, “Apparently, they can make an artificial womb, and that’s what they’re doing, and when they’re all done growing this baby, he’s going to come out of the hospital, he’s going to be OK, and it doesn’t seem to matter that they were born 16 weeks too early,” which sounds ludicrous. Of course it matters.
I wanted to believe in the stories of positive outcomes, but I also was very aware that we were facing a long road, and tried to prepare myself for being the mother of a child with disabilities.
How did your feelings change as Evan progressed and grew within the hospital setting?
I found myself with surprisingly strong protective instincts. No matter what fear I had initially about what it meant to have a baby born that early, I fell in love with my son, and it was my job to be his mother, and it was my job to learn how to be his mother, whatever those challenges might be.
What advice do you have to other parents of super-preemies?
When your child is born this early, and they’re in the hospital, it’s really not your baby. The baby somehow belongs to the doctors and the team. It’s not up to you to provide the care that that child needs.
But even given the fact that you’re not responsible for that level of care, you can become the advocate who learns and knows everything there is about this situation, and potential difficulties that you may face. I think it’s very important to stare those down, and to learn what they may be, because when you come home you need to be as prepared as possible.
When Evan finally did get out of the hospital, what problems did he face?
My son came home with 15 different diagnoses, and at least half a dozen medications that he required on a regular basis, and referrals to half a dozen specialists. Taking care of him became a full-time job, and I certainly applied myself to those duties with as much diligence as I’ve applied myself to anything in my life.
Did you feel like the risks of extreme prematurity were clear to you before you had the twins?
My husband and I did go through fertility treatments, and the multiple birth was the result of those fertility treatments. I remember in passing the doctor mentioning multiple birth as a potential “risk,” as he put it, but never mentioning prematurity or extreme prematurity as a subsequent risk.
I think that fertility doctors clearly are very focused on providing a successful pregnancy for their patients. And parents who want these children are also very focused on achieving a successful pregnancy. It’s not a story that one wants to hear. I don’t know if someone had told me that this was possible that I would have even been prepared to listen. But it is a reality, and it does happen.
I’m not a statistician, but we’re seeing more fertility treatments, which result in more multiple births. And multiple births carry a much higher risk of prematurity — that’s a fact.
As you were going through the initial months of your son’s life, how did your friends and family react?
It was unpredictable. The people who I thought would be by our side and understand weren’t always the people who were able to know what to do. This experience affects an entire family and circle of friends in ways that you can’t describe, and some friends were very supportive, and some friends were overwhelmed, and really didn’t know how to handle it.
I think that it’s a very challenging experience. I think it’s hard on everyone. It’s hard on family, and it’s hard on friends. I don’t think that people are equipped always to know what to do or say.
What advice do you have family and friends?
I think that the best advice is to maintain contact, and to simply say: “What can I do?” And if the answer is “nothing,” then keep calling and say: “What can I do? Is there anything I can do?”
The hardest part for me during this entire experience when Evan and Ellie were born, during those years of his chronic illness, was just feeling alone. I think it’s really important for parents not to feel alone. So, whatever a family member or friend can do to make that person feel less alone that’s the thing that is going to make the difference. Not the right words.
Is it because you are so consumed with your child’s care that you feel alone? Or, because you didn’t have contact with other parents who were going through the same thing?
I think that it has more to do with the trauma of the experience. I think that anyone who has gone through trauma will say: “I can’t explain this. No one understands this.” It’s just the typical reaction to trauma. The people who make you feel less alone are the people with whom you share that trauma.
Do you think that the parents should have the ultimate say about intervening to save an extremely premature child’s life? Or that hospitals should just be more clear about their policies upfront?
I think that the parents should have the final decision, and I think that that decision needs to be informed by some honest facts about outcome. It’s a terrible decision, but it really has to be for the people who are going to be living with their children, and caring for them for the rest of their lives. Those are the people who have the right to make the decision ultimately.
What do you mean by the honest facts about outcome?
Ninety percent of babies born about Evan and Ellie’s gestational age have permanent disabilities of some kind. I knew that, because I had done my research, and I said that during the delivery, and I think the doctor was trying to convince me that wasn’t true.
A lot of people would not know that, and then hear the stories about the 24-weeker who is just fine, and go home very unprepared. There are a range of permanent disabilities — learning disabilities, blindness — but these are lifelong disabilities, and that is the reality.
What were some of the disabilities that your son had?
My son was blind. He did walk eventually at the age of 5, but he was very obviously developmentally delayed in terms of his walking. He was nonverbal. He did not really eat. He came home with a permanent feeding tube. For several years, we fed him solely through that feeding tube. Eventually he did learn to drink a little, and take a little bit by mouth, but he was never going to eat hamburgers and hot dogs.
He had very low muscle tone, which made it hard for him to achieve any kind of developmental milestones. He didn’t smile until he was 9 months old, which most parents would know is very delayed.
But you came to see not only in these clinical terms, because he was your son, and you could experience his joy as well.
I did. He taught me how to see his life as a real life. I’m grateful that I was able to learn that lesson.
After he was out of the initial extreme crises, do you feel like he had good quality of life?
Absolutely. He was loved. He was cared for. He was happy.
At what point were you able to feel like you weren’t in a constant state of emergency when it came to his health?
Every time he got sick I was in a renewed state of emergency. It was relentless from the time he was born until about the time he was 3 years old.
The first two years were especially difficult. We were seeing doctors all the time, he was sick all the time. He was on medication. He remained on oxygen. We had a lot of medical supplies in the house. My dad came to visit me, and he said: “You’ve got your own little ICU here,” and he was right.
But after about 2 years, gradually we’d find ourselves with a little less to worry about. And by the time he was 3 he was no longer fragile or chronically ill.
How did your son’s condition impact his older sister?
My daughter from the time Evan came home until many years later would want to play these games that I thought were just sort of normal play, and now looking back I see that she was really working a lot out. We would play the patient game. She would hook me up to machines, as she called them, using yarn, and then I would have tubing. And then she would give me shots.
She certainly missed her sister. She thought she was going to have a sister, and she doesn’t. I think also she was afraid. When something like this happens, a child automatically worries that it could happen to them. I did what I could to be present for her, while also being very aware that her life had changed in a significant way, and there was nothing I could do about that.
How did this experience affect your marriage?
My husband and I would find new things to fight about. Like any marriage, we had had our ups and downs, we’re very solid, and we’re still solid, but I think that this experience puts such a strain on a marriage, and there is no avoiding that strain.
Eighty percent of couples with disabled children divorce, and we knew that statistic. We worked hard. We still work hard. And we certainly had to solve problems in our marriage that many people do not have to solve, such as where do we bury our child? Or, I don’t feel like taking him to the 15th doctor’s appointment this week, can you do it? Those kinds of negotiations were certainly far more intense than most people have to make in a marriage, but we’ve made them, and so we’re lucky.
Initially, you blamed yourself for the twins’ extreme prematurity. Why do you think you did that? And how did that change over time?
I think as mothers we feel very omnipotent, and very responsible, as though we’re supposed to somehow make everything go well. And in my case I had not been able to do that, so I felt responsible. A lot of people tried to explain to me that it wasn’t my fault.
But I still felt as thought I should have known, and I should have been able to prevent it. Finally, I understood that I had to stop blaming myself, and accept what happened, and that it wasn’t my responsibility. That is humbling, because the other side of the belief in your omnipotence is the realization that maybe you’re not in charge.
What were your experiences like with doctors who treated your son?
I think that we were left behind by doctors who felt that a normal outcome was a child who could see and talk and walk. And that we did not have that. It took me a long time to understand that there were some doctors who were going to walk away and say: “That one didn’t work out.”
But that there would also be some doctors who would say: “Look at him. Look at what he’s doing. This is amazing,” and feel like that was more important.
What was your son’s life like from ages 3 to 8?
When my son was 3, like most children with disabilities, he entered special education. He went to a very small, public special ed classroom, preschool. He had devoted teachers and therapists who saw him through so many personal challenges.
He had a lot of really big successes. He learned how to walk. He did learn how to feed himself a little bit. He was happy. He loved his friends. He laughed.
Kids in preschool have to stand up and put their little name on the felt board and say: “I’m here.” And he would stand up, and put his name up. Then he had this assistive technology, a button he could push that said, “I’m here.” And he would laugh, and think that was just so great.
How did Evan ultimately die, and why?
On the morning of his death, my son woke up happy and playful. He had been experiencing some discomfort that we weren’t able to really problem solve, because he was nonverbal.
But by noon, he had developed an acute abdominal obstruction, and by 2 the next morning he had died, due to organ failure essentially brought on by this obstruction. It was shocking and tragic and utterly unexpected.
As we later learned, the obstruction actually dated back to the surgery that he had had to place his permanent feeding tube. So, in effect, my son died from complications from his prematurity.
How do you feel you were changed by having the twins?
I think that I understand better now that you can feel more than one way at a time about something. We live in this very either-or culture. Either it’s a miracle or we’re a success, or we’re somehow a failure, and we’re not a miracle.
But in my own experience, I could want not to resuscitate my twins, and I could love them. I could be my son’s mother, and I could understand how to be the parent of a disabled child, and I could feel joy again. For me, it’s just been very eye-opening to see that you can feel both ways, and there is sorrow in the joy. I learned how to hear not loss but life.
———-
Do you have experience raising or caring for a child with a disability? Share your stories on Open Salon — click here for more details.