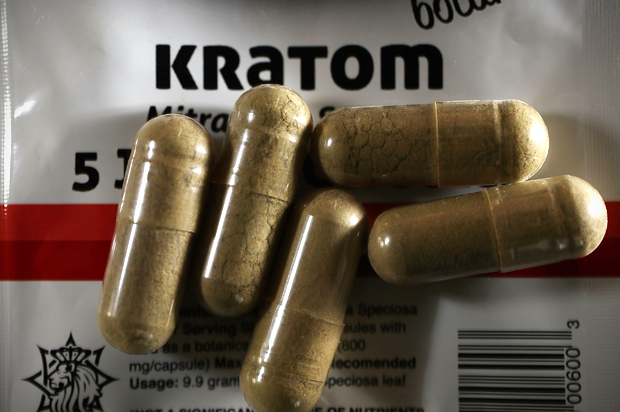
Given the opioid addiction crisis, it would seem preposterous that an opioid is legal for use in the United States and can be purchased at tea stores, convenience stores, over the internet and, yes, even from vending machines.
However, kratom is not your average opioid. The Drug Enforcement Agency found this out when it tried to ban the herb in 2016.
Public outcry from users and 51 congressmen around the country from both political parties was loud. The DEA has since dropped its attempt to ban kratom, although its use is banned in Alabama, Arkansas, Indiana, Tennessee, Vermont, Wisconsin and Louisiana.
More recently, on Nov. 14, 2017, the FDA issued a public warning about kratom, citing 36 deaths that the agency has attributed to kratom use.
Kratom lies at the intersection between natural product and drug of abuse, areas I have been been exploring as a clinical pharmacology researcher and a pharmacist for two decades. From ephedra for weight loss to MDMA (molly) for PTSD, experience has taught me that natural products are not always safe and that banned drugs may actually benefit some patients.
A popular plant
Thousands of people take kratom, which grows naturally in Thailand, Malaysia, Indonesia and Papua New Guinea, to relieve pain, believing a natural herb to be safe. However, we just do not know enough about the herb to deem it safe, or effective.
We do know that kratom has very mild pain-relieving effects and a slight stimulant effect. It brings a low risk of stopping breathing, the main risk of stronger opioids.
The opioid effects from kratom come from two potent chemicals, mitragynine and 7-hydroxymitragynine in kratom’s leaf. Mitragynine is the more prominent and has very mild opioid effects, while 7-hydroxymitragynine is 13 times more potent than morphine milligram for milligram.
But just because kratom is not as dangerous as heroin and fentanyl does not mean it is free of adverse effects. In fact, they are all highly addictive.
In an assessment of the 660 calls about kratom to United States poison control centers from 2010-2015, the major adverse effects included racing heartbeat, agitation or irritability, drowsiness, nausea and high blood pressure. The adverse effects were moderate or severe in 42 percent and 7 percent of people, respectively.
In addition, unlike prescription drugs, the quantities of the active ingredients in unregulated kratom products can change over time or can be adulterated with other products. In an assessment of several kratom products commercially sold in the Western world, the concentrations of 7-hydroxymitragynine were substantially higher than could be achieved naturally, which negates the safety benefits of using kratom versus other opioids.
Help for hard workers?
Kratom has been used widely in Southeast Asia for millennia, but it was banned in Thailand in 1943. Fans of the herb said the ban was due to politics, not health.
The ban hardly stopped its usage there. According to the 2008 national survey in Thailand, more than a million people reported using kratom. In several southern districts in Thailand, up to 70 percent of the male population reportedly uses kratom daily.
In Malaysia, the majority of people reported use of kratom to enhance their ability to work long hours with less pain and fatigue, but 31 percent began out of curiosity or peer pressure. Fifteen percent reported using kratom to wean off illicit drugs and alcohol. Eighty-nine percent of subjects tried to abstain from kratom in the past but all had relapsed due to withdrawal symptoms, such as insomnia, nausea, vomiting, diarrhea, muscle pains and shakiness, runny eyes and nose, anxiousness, depression and tension.
In the U.S., kratom’s safety profile – at least compared to other opioids – led people as far back as 1836 to recommend kratom as a substitute for people who became addicted to opioids. This belief was the main reason for the outcry against the proposed DEA ban in 2016. Despite the internet hype and extensive anecdotal experience, I do not think there any high-quality studies assessing how well it actually works and the best ways to use it.
Keeping quiet
A small study in Malaysia of 136 kratom users in 2010 suggested that kratom was effective at reducing the use of opioids. But, of the 78 percent of the respondents who subsequently tried to quit using kratom, none was successful.
We already have drugs that can be used for opioid addiction, including suboxone and methadone, which have been rigorously studied but also are addictive. It is reasonable to ask: Why would someone use kratom to help treat addiction?
Kratom offers something that other drugs to treat addiction do not – the ability to treat oneself in anonymity and to receive treatment without involving the health care system or law enforcement.
We need more information. Having the DEA ban a product makes the scientific inquiry into that product extremely difficult. This has impaired researchers’ ability to sensibly investigate the medicinal properties of marijuana, to the detriment of patients, I believe.
What is the bottom line?
Kratom is a promising option as an effective and safe substitute for people addicted to prescription opioids, which needs to be explored.
At the same time, kratom has high addiction potential and is risky when combined with other psychiatric drugs or drugs of abuse. Having kratom available to purchase in nearly unlimited quantities in venues that do not restrict purchase by age is a very bad idea.
A middle ground between this Wild West policy and a ban on kratom is to establish it as a third class of drugs. In 2006, Congress passed a law moving decongestants (pseudoephedrine, ephedrine and phenylpropanolamine) from over-the-counter to behind-the-pharmacy-counter status.
That law limits the monthly amount of the decongestants any individual could purchase. It also limits the sale to adults with photo identification and requires retailers to keep personal information about these customers for at least two years after purchase. Congress could pass a similar law for kratom and even place further restrictions, such as requiring kratom products to contain a standardized amount of the active constituents and that patients provide a medication history to the pharmacist, who can check for harmful drug-drug interactions and counsel patients on safer ways to use the drug.
![]() As with decongestants, this can be done efficiently and discreetly, because there are over 275 million patient visits to places that have pharmacies in them in the United States each week.
As with decongestants, this can be done efficiently and discreetly, because there are over 275 million patient visits to places that have pharmacies in them in the United States each week.