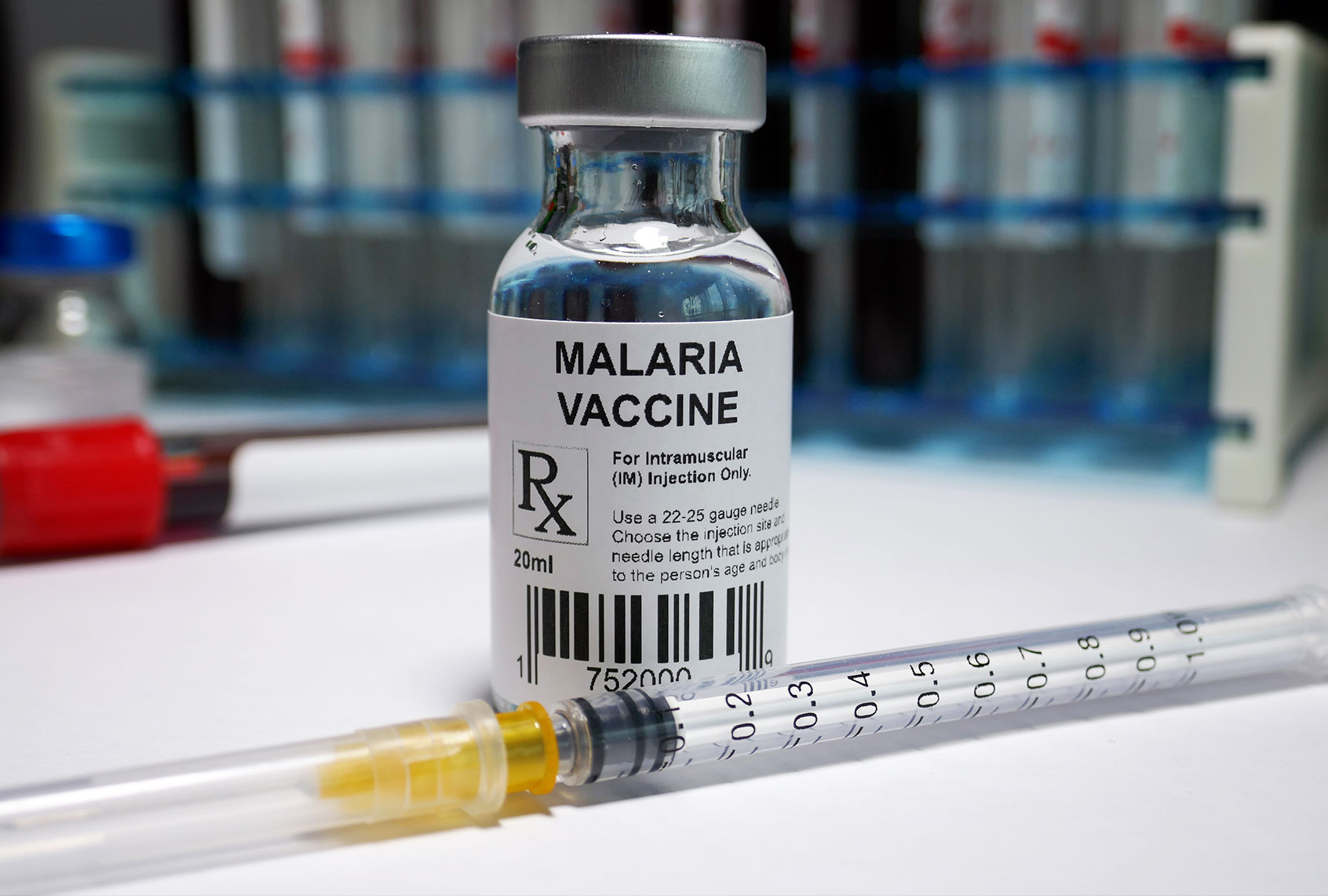
On Wednesday, the World Health Organization (WHO) recommended a broad rollout for a malaria vaccine after a pilot test showed that it was safe and could be effectively deployed in rural settings. Their historic announcement marks a turning point in the fight against malaria, as the first vaccine to exist for the disease that killed an estimated 400,000 people in 2019 (the most recent year for which updated data is available). Most deaths from malaria occur in sub-Saharan Africa; more than half of those deaths in 2019 were children under the age of 5.
The vaccine, dubbed RTS,S/AS01 (RTS,S) and also named Mosquirix, was made by GlaxoSmithKline. According to the pilot study’s results, the vaccine is 30 percent effective in reducing the risk of severe malaria, and 40 percent effective in reducing the risk of contracting malaria.
“This is a historic moment. The long-awaited malaria vaccine for children is a breakthrough for science, child health and malaria control,” said WHO Director-General Dr Tedros Adhanom Ghebreyesus. “Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year.”
The vaccine is administered as a series of four shots when a baby is between five to six months old. The first three are given each a month apart. Then a fourth is administered nearly a year later when the child is nearly two. To date, more than 2 million shots have been administered in the vaccine’s pilot program to more than 800,000 children in Ghana, Kenya, and Malawi; very few serious side effects have been reported.
Notably, WHO’s stamp of approval doesn’t mean widespread vaccine access. The next step, WHO says, “will include funding decisions from the global health community for broader rollout, and country decision-making on whether to adopt the vaccine as part of national malaria control strategies.” The vaccine costs about $5 a dose.
“For centuries, malaria has stalked sub-Saharan Africa, causing immense personal suffering,” said Dr. Matshidiso Moeti, WHO Regional Director for Africa. “We have long hoped for an effective malaria vaccine and now for the first time ever, we have such a vaccine recommended for widespread use. Today’s recommendation offers a glimmer of hope for the continent which shoulders the heaviest burden of the disease and we expect many more African children to be protected from malaria and grow into healthy adults.”
The announcement comes at a time when vaccines are clearly on the public’s mind amid a global pandemic for a different disease, COVID-19. Yet unlike the COVID-19 vaccine, which was created in little more than a year after discovery of the SARS-CoV-2 virus, malaria has been known to humans since the dawn of recorded history; it is mentioned in texts from India’s Vedic Period (1500–800 BCE) and in Homer’s “Illiad” (~750 BCE).
Given how long humans have been studying malaria, it is reasonable to ask why has it been so difficult to develop a vaccine for malaria — and why, in contrast, the vaccine for SARS-CoV-2 was developed at such a fast pace.
Want more health and science stories in your inbox? Subscribe to Salon’s weekly newsletter The Vulgar Scientist.
Part of the answer lies in the nature of the diseases. Malaria is a parasite, not a virus like SARS-CoV-2, or influenza. Unlike a virus, parasites are far more complex.
“The malaria parasite is a complex eukaryotic organism; it has 5,000 genes, and the coronavirus has less than 10 genes,” Dyann Wirth, who chairs WHO’s Malaria Policy Advisory Group and is a professor at Harvard’s T.H. Chan School of Public Health, explained to Salon. “In the case of malaria, the organism has 5,000 genes, so just to give you a sense, that’s as many genes as, say, a yeast organism.” Wirth noted that the malaria parasite is “a full independent living organism, with all the bits that it needs — whereas viruses invade a cell, and can’t actually replicate on their own.”
In other words, viruses like SARS-CoV-2 don’t live independently; they replicate only vis-a-vis the host’s cells. But in the case of malaria, the organism is alive on its own. (Most biologists don’t consider viruses to be “alive” in the technical definition of the word.)
“Parasites are sort of an adaptation of eukaryotic organisms where they have that same complexity, but they’ve evolved where they actually interact with the host and take some benefit from the host . . . they have all of their own machinery to replicate and to make proteins, and to make themselves available for transmission and so forth,” Wirth said.”So they need the host, but not in the in the same way that a virus does.” Wirth said this in part accounts for their increased complexity compared to viruses.
On top of this, Wirth said, the malaria parasite has been able to evolve for millennia and has become both advanced and smart. Malaria is caused by the Plasmodium parasite, which is injected into a human when an infected female Anopheles mosquito bites a person. The parasite migrates to the liver, replicates itself and infects the blood. This can cause a fever, chills and flu-like symptoms. While children can die from this due to their weaker immune systems, healthy adults usually recover. But in the case of developing a vaccine, the protein is hidden from the immune system until it gets to the liver.
“There’s kind of what I would say, a shield strategy,” Wirth said. “And if you take and compare malaria parasites, you’ll find dozens of genes that are different, even between parasites that are circulating the same at the same time and in the same part of the world, and this antigenic diversity allows the organism to escape the human immune system as a population, not as an individual parasite.”
Unlike many viruses, malaria can infect a human host more than once. Once it gets to the liver, it expresses a whole new set of proteins, creating essentially a new infection.
This, in part, is why the efficacy of the new malaria vaccine is low compared to the SARS-CoV-2 vaccines.
“Unlike a viral vaccine, where the vaccine gets lots of shots on goal or the immune system gets lots of shots on goal, for malaria, for the invading stage, there’s only one shot,” Wirth said. “It’s a binary thing, the infection is either prevented or it’s not.”
Plus, Wirth said, with the COVID-19 vaccines, billions of dollars and hundreds of people were working tirelessly on development.
“There were 135 [COVID-19] vaccine candidates, in the entire history of malaria vaccine research there’s maybe been five or so, or maybe 10, but there hasn’t been that same kind of investment,” Wirth said. “Would it have been successful? Hard to say, but certainly trying everything that you can imagine, all at once, did have an accelerating effect on the field.”
So, how does that malaria vaccine work? Rather than target the parasite itself, the vaccine targets the sporozoite protein that helps the parasite find the liver.
“The vaccine induces an antibody which prevents the sporozoite from invading the liver,” Wirth explained. “So it’s very much like the coronavirus vaccine or the flu vaccine, because it’s an antibody to a protein that’s found on the surface of the organism, which just prevents it from interacting with its host receptor.”
Wirth said she hopes the success of these vaccines will guide the scientific community into a new era of vaccine development.
“I hope it will unleash what will be a renaissance of thinking,” Wirth said.