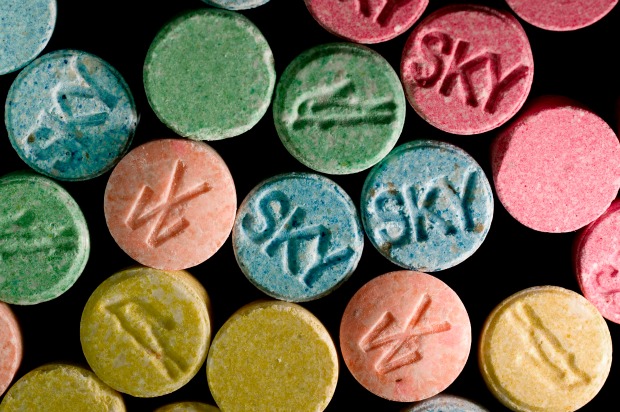
Given the highly anticipated legalization of marijuana in several states, including New York in January 2016, some activists think it’s high time that Americans also reconsider the use of other Class I drugs for therapeutic purposes: in particular, MDMA and Ayahuasca for the treatment of veterans with PTSD.
Just in time for Veteran’s Day, Brad Burge, director of nonprofit research and educational organization MAPS (Multidisciplinary Association for Psychedelic Studies) is leading a live webseminar discussion on MDMA and Ayahuasca in a medicinal context today with former Marine Ryan LeCompte, as part of MAPS’ “Psychedelic Science and Spirituality” series. LeCompte, who says he successfully recovered from PTSD with the help of psychedelics, founded the veteran’s support group VET (Veterans for Entheogenic Therapy) and is currently planning an Ayahuasca observational study partly funded by MAPS.
7.8 percent of all Americans will, at some point, suffer from PTSD, along with 10 percent of all Gulf War veterans and 11 percent of Afghanistan veterans, as our society feels increasingly alienated by and numbed to current events like extended combat and terrorism.
When I spoke to Burge, he emphatically referred to PTSD as an “epidemic,” citing the historically unprecedented rise of the anxiety disorder among the general American population, as well as the proven ineffectiveness of FDA-approved drugs: “What the currently approved medications for PTSD do is they mute or dull the symptoms. People have to take these drugs everyday the rest of their life, and even then a third of them don’t get better at all. You’re not getting at the deeper issue, which is somebody’s relationship with their traumatic memories.”
But there is hope in the results of new medical research involving MDMA. According to MAPS, its Phase II study of treating PTSD with MDMA saw an 83 percent success rate compared with that of conventional therapy, which is approximately 20 percent; and that’s often after only two sessions of actual MDMA-assisted psychotherapy.
I spoke with LeCompte about stigma inside and outside the Marine Corps, as well as his personal struggle to find proper mental care, and ultimately, spiritual healing.
Ryan, after you were diagnosed with PTSD in the Corps, did you receive medical treatment relatively swiftly? What kinds of medication did they prescribe for you?
On active duty, the mental health programs are crap, and at the VA — they are outstretched. Right now there are more veterans in care for mental illness than physical disabilities. So it would be advantageous of the VA to consider alternative treatments because it would help the budget deficit.
It didn’t take more than a month to get prescribed three types of medication for my PTSD symptoms. The first was antidepressants — I was prescribed Prozac. I think it’s effective for short term, but the way they were prescribing it for me and a lot of other veterans seemed to be their long term solution. I also had Klonopin for anxiety. The third was Ambien for sleep issues. They’re starting to call it “a cocktail of disaster.”
So was the doctor who prescribed you this “cocktail” aware of the effects of mixing these medications together?
That’s what baffled me. You’re an MD psychiatrist and you’re prescribing contra-indicated substances at the same time? After a month and a half of taking these and becoming a zombie, I was like “No.”
What actually led you to explore psychedelic drugs as a therapeutic alternative?
I met a friend at community college and we did underground psychedelic therapy together. That was the first time I got introduced to psychedelics. I just thought they were something that happened in the ‘60s when a lot of people put flowers in their hair and danced crazy.
Then I smoked DMT and got some clear visions, spiritual visions, and started doing the scientific research.
It led me to create my nonprofit group called VET, Vets for Entheogenic Therapy, to gather around Ayahuasca and DMT. We have almost 3,000 members now and they’re all vets who were saying, “We want something different. We want to try Ayahuasca.” So I just responded to that. From that I started working with MAPS and gave them a proposal to look into an observational Ayahuasca study for treating PTSD.
Brad Burge from MAPS mentioned that you were organizing an Ayahuasca trip to Peru for treatment-resistant veterans with PTSD — can you tell me a little bit more about it?
So the trip will involve twelve veterans diagnosed with PTSD from the Boulder area. Originally we were supposed to go to a center in Peru, but they said “We don’t have the capacity for holding combat vets with PTSD.” So I found this church in Florida called ONAC. They’re a Oklevueha Native American Church, which is legally allowed to serve Ayahuasca under the Religious Freedoms Act.
What sort of policy changes or drug law reforms would you like to see happen in the near future?
Marijuana’s the gateway to psychedelics and ayahuasca, so I support the marijuana movements. What I’d like to see happen in a post-Prohibition world is more harm reduction models come out at festivals, and for the federal government to grant psychedelic licenses to medical professionals who want to work with it in their practice.
So experientially, what’s it like recovering from PTSD using psychedelics?
For a lot of other veterans and myself, Ayahuasca works the same way that exposure therapy does. They distract your mind while they ask you to recall the traumatic event — it’s like bifurcating your consciousness so that you can cathart the memory.
But for treatment-resistant vets, it’s hard because you get all the emotional stuff that comes up with recalling the memory. So Ayahuasca actually targets that part of the brain, the amygdala, which is responsible for fight or flight, as well as the serotonergic system which is responsible for happy feelings.
The spiritual side of Ayahuasca helps you make meaning of the traumatic event. You start to see how the trauma can be reassessed back into your life in a way that can be productive, versus feeling like a victim.
Did you personally find Ayahuasca more effective for treating your PTSD than MDMA?
MDMA deals more with psychological processing, so it works well when you want to build the ego back up and connect within on a more existential level. Ayahuasca is more of an ego dissolution involving intense out-of-body experiences and visual hallucinations, where you become — I know this is really weird-sounding — everything around you. You have to have a strong ego intact to be able to take something like that. So Rick Doblin from MAPS and I were talking about how MDMA should be done before and after Ayahuasca, to reintegrate the experience.
Interesting. Did you happen to experience any negative side effects during your own psychedelic treatments?
Nothing other than the spiritual crisis. After drinking Ayahuasca in the Amazon with other vets, we had this awakening — when we got back to our daily lives, how were we going to integrate these experiences? That’s been my main struggle.
As a Marine, what do you think Americans need to know about vets with PTSD?
Part of the veterans’ transition struggle is becoming worldly and then coming back to a bubbled society that doesn’t understand what’s going on out there. We’re constantly being generalized as men and women who just signed up to kill people. We signed up to serve, and that part of it is being shunned out of the public view because of the war, because of the ambiguity around oil and the U.S.’s motives. I also see where we’re dirty too. We didn’t go in there just to spread freedom. Our government turned their backs on us, and the people did too, in a way. So we’re stuck in the middle.
In your opinion, does this macho culture within the military often make it harder for Marines to admit that they’re suffering from PTSD?
On active duty it’s hard to talk about because it’s the elephant in the room. When you’re back in the States, you just drink. I and a friend who got back from Iraq, Sergeant Leon Alcabar, drank a lot in the barracks; we were self-medicating. Leon didn’t feel like he could talk to the battalion psychiatrist about his issues because a lot of us were getting separated for “failure to adapt.” We could get kicked out under a med sep with no benefits for our families, and we were like, “No, we’re not going to do that.” So we just drank, and Leon decided he’d had enough and hanged himself in his barracks room. I found him the morning after when he didn’t show up for muster.
And that was my first real “stop — wait, what’s happening?” when I lost Leon. It just gets into the nature of PTSD — that macho syndrome of we’re warriors and not scared of death, and if we can’t talk about it, we’ll destroy ourselves.
Can I ask you if Marines commonly self-medicated while on active duty?
Yeah. It’s hard because you’re in a system that’s like a very tight-knit fraternity. The more the drinking happened, the more groupthink went on, the more command was coming down on Marines for disclosing information like “Oh, I’m having some issues around drinking.” It was really bad.
And then we all started smoking spice, because we didn’t want to bomb on a piss test, and that seemed to work. But then again, it was synthetic marijuana, so they started making it illegal in the Marine Corps and you could be court-martialed for it. It’s ridiculous. They became aware of spice before they became aware of a PTSD problem.
I was surprised to learn that a disproportionately high amount of U.S. veterans suffer from PTSD compared to their British and European counterparts. Why do you think that is?
Canada and Israel have specifically addressed it even earlier than the U.S. has. Canada has had a medical marijuana program for PTSD for a long time, and they’re about to legalize next year. Israel actually gives medical marijuana to active duty soldiers. So we’re kind of behind the times.
Finally, MAPS estimates that MDMA will be legalized by 2021. So I’d love to ask you: how long do you think it’ll take before the FDA approves Ayahuasca as a prescription drug?
Ayahuasca’s got a long way to go. While the veterans are doing their integration, I’ll be following up with them every three months using psychometrics like CAPS, which is a clinician-administered PTSD scale and the gold standard used by the VA. I’m hoping to see a significant drop in the scores by the end of the year. Once the study is done, we’re looking to take those results to the FDA and say, “Look, we have measurable behavioral effects that reduce symptoms of PTSD in treatment-resistant veterans.” If we do get FDA approval, Ayahuasca will be legal in about 20 to 25 years.