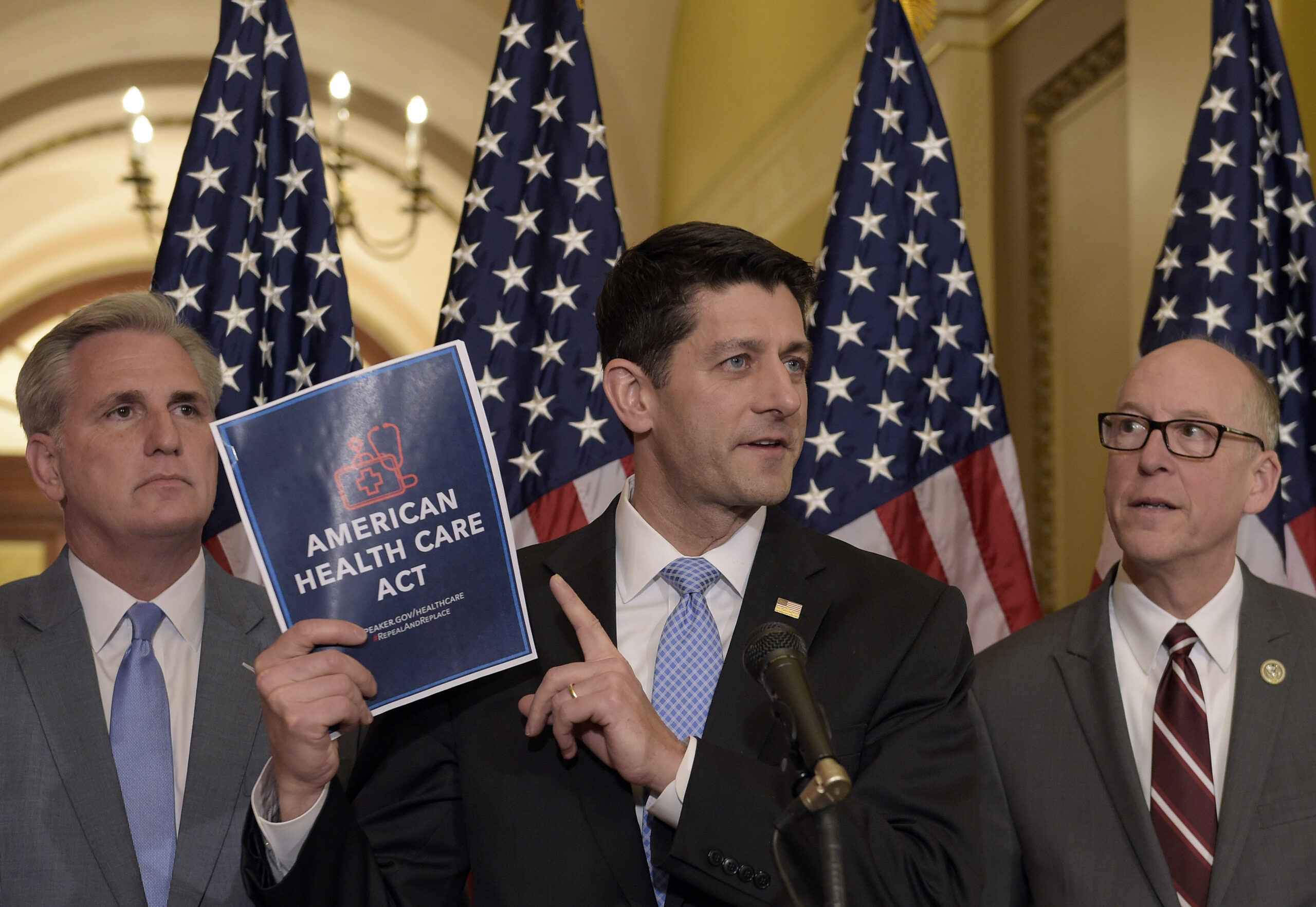House Republicans introduced the American Health Care Act (AHCA), their proposal to repeal and replace the Affordable Care Act (ACA, also known as Obamacare). ![]()
At a press conference, Speaker Paul Ryan called this bill “an act of mercy.” For the most vulnerable, that characterization is ironic at best.
Yes, there are winners in this bill. But those who benefit would be predominantly young, healthy and less likely to need insurance or older, well off and more likely to be able to afford insurance.
The potential effects of this bill on certain segments of the population are clear: For the millions of Americans with multiple chronic conditions, and for nearly 100 million Americans who earn less than US$40,000 a year, AHCA would bring less coverage and higher costs than under the ACA.
A quick review
First, it’s important to understand how much the ACA has helped Americans afford health insurance coverage. In 2009, 15.1 percent of Americans were uninsured. By 2015, that number had fallen to 9.4 percent.
Those who gained coverage did so primarily through the expansion of Medicaid and through the ACA’s health insurance marketplace. These coverage expansions have provided crucial assistance to low-income Americans, many of whom were unable to afford coverage before the ACA.
Today, adults with incomes up to 138 percent of the federal poverty level, or about $16,394 in 2017, are eligible to enroll in Medicaid in the 32 states, including the District of Columbia, that expanded the program.
The law had originally intended for all states to expand their Medicaid programs; a 2012 Supreme Court ruling made the expansion a state option. People with incomes up to 400 percent of the federal poverty level, or $47,520 in 2017, can get financial assistance to purchase coverage on the Health Insurance Marketplace.
In 2016, nearly 9.4 million people – 85 percent of Health Insurance Marketplace enrollees – received tax credits to help pay for premiums.
In addition, under the ACA, individuals with incomes less than 250 percent of the federal poverty level, or $29,700 in 2017, receive cost-sharing reduction subsidies to help pay for copays and deductibles.
Almost 6.4 million people – 57 percent of 2016 Health Insurance Marketplace enrollees – received these subsidies to help lower their out-of-pocket costs. The cost-sharing subsidies helped people to afford health care as well as insurance coverage.
Presidential promises for insurance for everyone – and cheaper
Over the past several months, President Trump has promised an ACA replacement plan that will provide “insurance for everybody” that is “much less expensive and much better” with “much lower deductibles.”
Those promises are good benchmarks to help us evaluate the impact of the American Health Care Act.
In its current form, the AHCA simply does not accomplish any of those goals for people with low incomes, people over 60, or people who live in areas where health care costs are high, such as rural areas. Indeed, the AHCA may end up putting health coverage out of reach for many of those who gained it under the ACA.
The AHCA replaces the ACA’s income-based premium tax credits with age-adjusted tax credits (with an income limit of $115,000). Under the AHCA, adults in their 20’s would receive a $2,000 annual tax credit to help purchase individual market coverage, with tax credits increasing up to $4,000 for a 60-year-old.
These proposed tax credits do not take into account an individual’s income or the price of health insurance in their area, as the ACA did. According to the Kaiser Family Foundation, the average annual premium tax credit in 2017 under the ACA for a 60-year-old making $20,000 a year was $9,874.
Under the AHCA, that same 60-year-old would receive less than half that amount, according to an analysis by the Kaiser Family Foundation. In many areas of the United States, particularly rural areas, older Americans would receive significantly less financial assistance to help pay for premiums than they currently receive.
Under the ACA, the premium tax credit amount that enrollees may receive is based on two key factors: the local benchmark premium cost and the enrollee’s household income. Under the AHCA, premium tax credits would be based only on age and would not be tailored to local costs.
The AHCA would also repeal the ACA’s cost-sharing subsidies in 2020, putting care even further out of reach for many.
The AHCA would expand those age bands so that older adults could now be charged up to five times higher premiums than their younger counterparts. Older adults could not only see a decrease in financial assistance to pay for premiums, but their premiums could increase as well.
More to the problem than Medicaid loss
For the 12 million people who are now covered through Medicaid expansion, the outlook is equally gloomy. The AHCA would freeze Medicaid expansion beginning in 2020. States that had already expanded the program would continue to receive enhanced federal funding for current enrollees who remain on the program.
But states would receive far less federal funding to cover any new enrollees or any existing enrollee who experiences a lapse in coverage longer than one month. Many states would find it difficult to continue Medicaid expansion under these circumstances.
In addition, beginning in 2020, the bill would shift Medicaid to a per-capita cap. This would be a fundamental restructuring of the Medicaid program, affecting over 70 million people.
Unlike today, where the federal government guarantees it will match states’ costs to provide care to Medicaid beneficiaries, a per-capita cap would give states a fixed amount of money per enrollee. The state would be responsible for any expenses beyond that amount.
According to the Center for Budget and Policy Priorities, the AHCA’s proposed Medicaid changes would shift $370 billion in costs to states over 10 years. As a result, states would try to contain costs by curtailing benefits or limiting enrollment in their Medicaid programs – not just in the expansion population, but across the board.
While House Republicans claim these changes will grant more flexibility to states to make innovations in their Medicaid programs, the proposed structure would likely end up cutting benefits for millions of adults and children as states scramble to fill the shortfall from fewer federal Medicaid dollars.
Perhaps the AHCA can improve coverage and lower costs, but the real question is: For whom?
For the young, healthy, and high-income earners, quite possibly. But for lower-income individuals, older adults, people living in rural areas and people who gained Medicaid coverage under the ACA, it seems unlikely that the AHCA is anything but a bad deal.
Megan Foster Friedman, Health Policy Analyst, University of Michigan