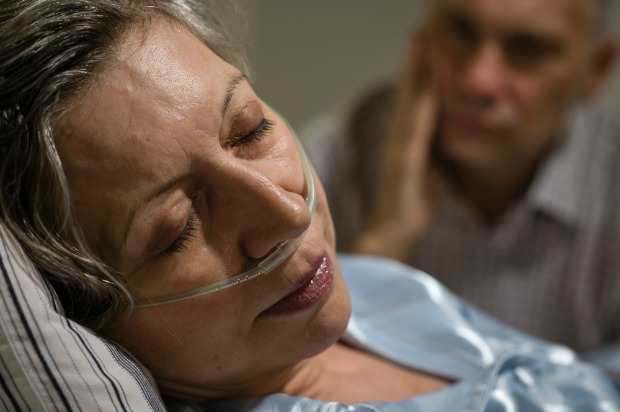
Gerald Chinchar isn’t quite at the end of life, but the end is not far away. The 77-year-old fell twice last year, shattering his hip and femur, and now gets around his San Diego home in a wheelchair. His medications fill a dresser drawer, and congestive heart failure puts him at high risk of emergency room visits and long hospital stays.
Chinchar, a Navy veteran who loves TV Westerns, said that’s the last thing he wants. He still likes to go watch his grandchildren’s sporting events and play blackjack at the casino. “If they told me I had six months to live or go to the hospital and last two years, I’d say leave me home,” Chinchar said. “That ain’t no trade for me.”
Most aging people would choose to stay home in their last years of life. But for many, it doesn’t work out: They go in and out of hospitals, getting treated for flare-ups of various chronic illnesses. It’s a massive problem that costs the health care system billions of dollars and has galvanized health providers, hospital administrators and policymakers to search for solutions.
Sharp HealthCare, the San Diego health system where Chinchar receives care, has devised a way to fulfill his wishes and reduce costs at the same time. It’s a pre-hospice program called Transitions, designed to give elderly patients the care they want at home and keep them out of the hospital.
Social workers and nurses from Sharp regularly visit patients in their homes to explain what they can expect in their final years, help them make end-of-life plans and teach them how to better manage their diseases. Physicians track their health and scrap unnecessary medications. Unlike hospice care, patients don’t need to have a prognosis of six months or less, and they can continue getting curative treatment for their illnesses, not just for symptoms.
Before the Transitions program started, the only option for many patients in a health crisis was to call 911 and be rushed to the emergency room. Now, they have round-the-clock access to nurses, one phone call away.
“Transitions is for just that point where people are starting to realize they can see the end of the road,” said San Diego physician Dan Hoefer, one of the creators of the program. “We are trying to help them through that process so it’s not filled with chaos.”
The importance of programs like Transitions is likely to grow in coming years as 10,000 baby boomers — many with multiple chronic diseases — turn 65 every day. Transitions was among the first of its kind, but several such programs, formally known as home-based palliative care, have since opened around the country. They are part of a broader push to improve people’s health and reduce spending through better coordination of care and more treatment outside hospital walls.
But a huge barrier stands in the way of pre-hospice programs: There is no clear way to pay for them. Health providers typically get paid for office visits and procedures, and hospitals still get reimbursed for patients in their beds. The services provided by home-based palliative care don’t fit that model.
In recent years, however, pressure has mounted to continue moving away from traditional payment systems. The Affordable Care Act has established new rules and pilot programs that reward the quality rather than the quantity of care. The health reform law, for example, set up “accountable care organizations” networks of doctors and hospitals that share responsibility for providing care to patients. They also share the savings when they rein in unnecessary spending by keeping people healthier. Those changes are helping to make home-based palliative care a more viable option.
In San Diego, Sharp’s palliative care program has a strong incentive to reduce the cost of caring for its patients, who are all in Medicare managed care. The nonprofit health organization receives a fixed amount of money per member each month, so it can pocket what it doesn’t spend on hospital stays and other costly medical interventions.
‘Something That Works’
Palliative care focuses on relieving patients’ stress, pain and other symptoms as their health declines, and it helps them maintain their quality of life. It’s for people with serious illnesses, such as cancer, dementia and heart failure. The idea is for patients to get palliative care and then move into hospice care, but they don’t always make that transition.
The 2014 report “Dying in America,” by the Institute of Medicine, recommended that all people with serious advanced illness have access to palliative care. Many hospitals now have palliative care programs, delivered by teams of social workers, chaplains, doctors and nurses, for patients who aren’t yet ready for hospice. But until recently, few such efforts had opened beyond the confines of hospitals.
Kaiser Permanente set out to address this gap. Nearly 20 years ago, it created a home-based palliative care program, testing it in California and later in Hawaii and Colorado. Two studies by Kaiser and others found that participants were far more likely to be satisfied with their care and more likely to die at home than those not in the program. (Kaiser Health News, which produces California Healthline, is not affiliated with Kaiser Permanente.)
One of the studies, published in 2007, found that 36 percent of people receiving palliative care at home were hospitalized in their final months, compared with 59 percent of those getting standard care. The overall cost of care for those who participated in the program was a third less than for those who didn’t.
“We thought, ‘Wow. We have something that works,’” said Susan Enguidanos, an associate professor at the University of Southern California’s Leonard Davis School of Gerontology, who worked on both studies. “Immediately we wanted to go and change the world.”
But Enguidanos knew that Kaiser Permanente was unlike most health organizations. It was responsible for both insuring and treating its patients, so it had a clear financial motivation to improve care and control costs. Enguidanos said she talked to medical providers around the nation about this type of palliative care, but the concept didn’t take off at the time. Providers kept asking the same question: How do you pay for it without charging patients or insurers?
“I liken it to paddling out too soon for the wave,” she said. “We were out there too soon. … But we didn’t have the right environment, the right incentive.”
A Bold Idea
Dan Hoefer’s medical office is in the city of El Cajon, which sits in a valley in eastern San Diego County. Hoefer, a former hospice and home health medical director and nursing home doctor, has spent years treating elderly patients. He learned an important lesson when seeing patients in his office: Despite the medical care they received, “they were far more likely to be admitted to the hospital than make it back to see me.”
When his patients were hospitalized, many would decline quickly. Even if their immediate symptoms were treated successfully, they would sometimes leave the hospital less able to take care of themselves. They would get infections or suffer from delirium. Some would fall.
His patients were like cars with 300,000 miles on them, he said. They had a lot of broken parts. “You can’t just fix one thing and think you have solved the problem,” he said.
And trying to do so can be very costly. About a quarter of all Medicare spending for beneficiaries 65 or older is to treat people in their last year of life, according to a report by the Kaiser Family Foundation. (Kaiser Health News, which produces California Healthline, is an editorially independent program of the foundation.)
Hoefer’s colleague, Suzi Johnson, a nurse and administrator in Sharp’s hospice program, saw the opposite side of the equation. Patients admitted into hospice care would make surprising turnarounds once they started getting medical and social support at home and stopped going to the hospital. Some lived longer than doctors had expected.
In 2005, the pair hatched and honed a bold idea: What if they could design a home-based program for patients before they were eligible for hospice?
Thus, Transitions was born. They modeled their new program in part on the Kaiser experiment, then set out to persuade doctors, medical directors and financial officers to try it. But they met resistance from physicians and hospital administrators who were used to getting paid for seeing patients.
“We were doing something that was really revolutionary, that really went against the culture of health care at the time,” Johnson said. “We were inspired by the broken system and the opportunity we saw to fix something.”
Despite the concerns, Sharp’s foundation board gave the pair a $180,000 grant to test out Transitions. And in 2007, they started with heart failure patients and later expanded the program to those with advanced cancer, dementia, chronic obstructive pulmonary disease and other progressive illnesses. They started to win over some doctors who appreciated having additional eyes on their patients, but they still encountered “some skepticism about whether it was really going to do any good for our patients,” said Jeremy Hogan, a neurologist with Sharp. “It wasn’t really clear to the group … what the purpose of providing a service like this was.”
Nevertheless, Hogan referred some of his dementia patients to the program and quickly realized that the extra support for them and their families meant fewer panicked calls and emergency room trips.
Hoefer said doctors started realizing home-based care made sense for these patients — many of whom were too frail to get to a doctor’s office regularly. “At this point in the patient’s life, we should be bringing health care to the patient, not the other way around,” he said.
Across the country, more doctors, hospitals and insurers are starting to see the value of home-based palliative care and are figuring out how to pay for it, said Kathleen Kerr, a health care consultant who researches palliative care.
“It is picking up steam,” she said. “You know you are going to take better care of this population, and you are absolutely going to have lower health care costs.”
Providers are motivated in part by a growing body of research. A study published in January showed that in the last three months of life, medical care for patients in a home-based palliative care program cost $12,000 less than for patients who were getting more typical treatment. Patients in the program also were more likely to go into hospice and to die at home, according to the study.
Two studies of Transitions in 2013 and 2016 reaffirmed that such programs save money. The second study, led by outside evaluators, showed it saved more than $4,200 per month on cancer patients and nearly $3,500 on those with heart failure.
The biggest differences occurred in the final two months of life, said one of the researchers, Brian Cassel, who is palliative care research director at the Virginia Commonwealth University School of Medicine in Richmond.
One reason for the success of these programs is that the teams really get to know patients, their hopes and aspirations, said Christine Ritchie, a professor at UC San Francisco’s medical school. “There is nothing like being in someone’s home, on their turf, to really understand what their life is like,” she said.
A Home Visit
Nurse Sheri Juan and social worker Mike Velasco, who both work for Sharp, walked up a wooden ramp to the Chinchars’ front door one recent January morning. Juan rolled a small suitcase behind her containing a blood pressure cuff, a stethoscope, books, a laptop computer and a printer.
Mary Jo Chinchar was already familiar with Transitions because her mother had been in the program before entering hospice and dying in 2015 at the age of 101. Late last year, Gerald Chinchar’s doctor recommended he enroll in it, explaining that his health was in a “tenuous position.”
Chinchar, who has nine grandchildren and four great-grandchildren, likes to tell stories about his time in the Navy, about traveling the country for jobs and living in San Francisco as a young man.
He has had breathing problems much of his life, suffering from asthma and chronic obstructive pulmonary disease — ailments he partly attributes to the four decades he spent painting and sandblasting fuel tanks for work. Chinchar also has diabetes, a disease that led to his mother’s death. He recently learned he had heart failure.
“I never knew I had any heart trouble,” he said. “That was the only good thing I had going for me.”
Now he’s trying to figure out how to keep it from getting worse: How much should he drink? What is he supposed to eat?
That’s where Juan comes in. Her job is to make sure the Chinchars understand Gerald’s disease so he doesn’t have a flare-up that could send him to the emergency room. She sat beside the couple in their living room, its bookshelves filled with titles on gardening and baseball. A basket of cough drops and a globe sat on a side table.
Any pain today? Juan asked. How is your breathing? Are you more fatigued than before? Is your weight the same? He replied that he had gained a few pounds recently but knew that was because he’d eaten too much bacon.
Posted on the couple’s refrigerator was a notice advising them to call the nurse if Gerald had problems breathing, increased swelling or new chest pain.
Juan checked his blood pressure and examined his feet and legs for signs of more swelling. She looked through his medications and told him which ones the doctor wanted him to stop taking. “What we like to do as a palliative care program is streamline your medication list,” she said. “They may be doing more harm than good.”
Mary Jo Chinchar said she appreciates the visits, especially the advice about what Gerald should eat and drink. Her husband doesn’t always listen to her, she said. “It’s better to come from somebody else.”
A Nearly Impossible Decision
On a rainy January day, doctors, nurses and social workers gathered in a small conference room for their bimonthly meeting to discuss patient cases. Information about the patients — their hospitalizations, medications, diagnoses — was projected on the wall. Their task: to decide if new patients were appropriate for Transitions and if current patients should remain there.
It’s nearly impossible to predict how long someone will live. It’s an inexact algorithm based on the severity of their disease, depression, appetite, social support and other factors. Nevertheless, the team tries to do just that, and they may recommend hospice for patients expected to live less than six months.
That was the case with an 87-year-old woman suffering from Alzheimer’s disease. She had fallen many times, slept about 16 hours a day and no longer had much of an appetite. Those were all signs that the woman may be close to death, so she was referred to hospice.
Patients typically stay in Transitions about seven or eight months, but some last as long as two years before they stabilize and are discharged from the program. Others go directly to hospice, and still others die while they are still in Transitions.
The group turned its attention to an 89-year-old woman with dementia, who believed she was still a young Navy wife. She suffered from depression and kidney disease, and had been hospitalized twice last year.
“She’s a perfect patient for Transitions,” Hoefer told the team, adding that she could benefit from extra help. Another good candidate, Hoefer said later, was El Cajon resident Evelyn Matzen, who is 94 and has dementia. She had started to lose weight and was having more difficulty caring for herself. They took her in because “we were worried that it was going to start what I call the revolving door of hospitalization,” Hoefer said.
About eight months after she joined the program, Matzen sat in Hoefer’s office as he checked her labs and listened to her chest. Her body was starting to slow down, but she was still doing well, he told her. “Whatever you are doing is working.”
Bill Matzen, who accompanied his mom to the appointment, said she had started to stabilize since going onto Transitions. “She is on less medication, she is in better condition, physically, mentally, the whole nine yards,” he said.
Hoefer explained that frail elderly patients have fewer reserves to tolerate medical treatment and especially hospitalization. Bill Matzen said his mother leaned that the hard way after a recent fall. Though the Transitions nurse had come to see her, the Matzens decided to go to the hospital because they were still concerned about a bruise on her head. While she was in the hospital, Evelyn Matzen started hallucinating and grew agitated.
Being in the hospital “kicks her back a notch or two,” her son said. “It takes her longer to recover than if she had been in a home environment.”
A Changed Climate
Outpatient palliative care programs are cropping up in various forms. Some new ones are run by insurers, others by health systems or hospice organizations. Others are for-profit, including Aspire Health, which was started by former senator Bill Frist in 2013.
Sutter Health operates a project called Advanced Illness Management to help patients manage symptoms and medications and plan for the future. The University of Southern California and Blue Shield of California recently received a $5 million grant to provide and study outpatient care.
“The climate has changed for palliative care,” said Enguidanos, the lead investigator on the USC-Blue Shield project.
Ritchie said she expects even more home-based programs in the years to come, especially if palliative care providers work alongside primary care doctors. “My expectation is that much of what is being done in the hospital won’t need to be done in the hospital anymore and it can be done in people’s homes,” she said.
Challenges remain, however. In addition to questions about reimbursement, not enough trained providers are available. And some doctors are unfamiliar with the approach, and patients may be reluctant, especially those who haven’t clearly been told they have a terminal diagnosis.
Now, some palliative care providers and researchers worry about the impact of President Donald Trump’s plans to repeal the Affordable Care Act and revamp Medicare.
“It would be horrible,” Kerr said. “Before, we had an inkling that this was helping a lot of folks. Now we know it is really helping.”
Gerald Chinchar, who grew up in Connecticut, said he never expected to live into old age. His father, a heavy drinker, died of cirrhosis of the liver at 47. In his family, Chinchar said, “you’re an old-timer if you make 60.”
Chinchar said he gave up drinking and is trying to eat less of his favorite foods — steak sandwiches and fish and chips. He just turned 77, a milestone he credits partly to the pre-hospice program.
“If I make 80, I figured I did pretty good,” he said. “And if I make 80, I’ll shoot for 85.”
KHN’s coverage in California is funded in part by Blue Shield of California Foundation.