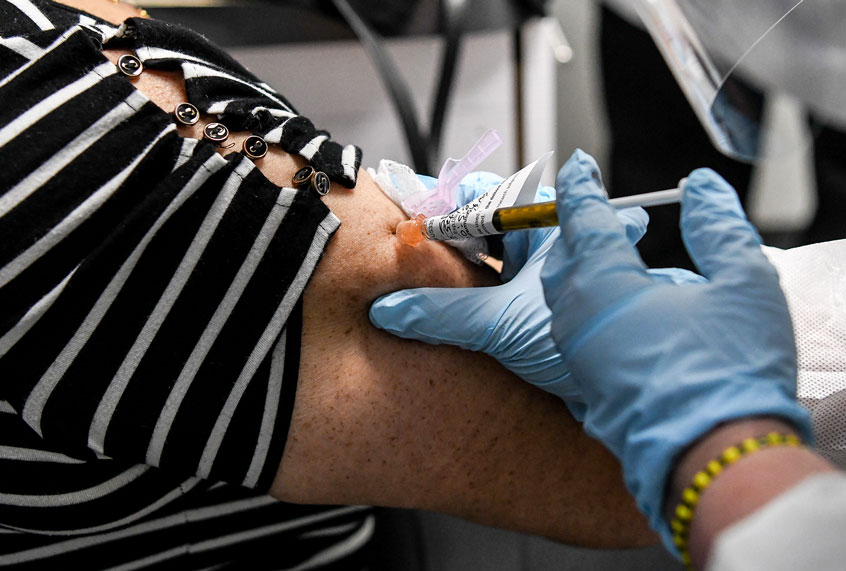
Imagine, after months of quarantining and avoiding contact, signing up to go into a sealed facility where a stranger in full-body protective gear deliberately infects you with coronavirus. This quarantine has made most of us deeply afraid of contracting COVID-19 — perhaps understandably given the horror stories and mortality rate. Yet tens of thousands of people around the world say they’d participate in what are known as “challenge studies” for coronavirus vaccines.
What’s a challenge study? In a regular vaccine trial, participants get the vaccine, and then researchers record how many of them get the virus anyway. In challenge studies, researchers give participants the vaccine, and then they also expose them to the virus, in a contained facility. The hope is that researchers could get data on the efficacy of the vaccine more quickly than they would with a standard trial. As of this writing, over 33,000 people from 151 countries have signed up on the website of a new public health nonprofit, 1 Day Sooner, to be part of a future challenge study.
A long roster of volunteers doesn’t mean that researchers can start challenge studies right away. They’d need to vet volunteers’ eligibility, and get their full informed consent, before the volunteers could become challenge study participants (or, as 1 Day Sooner’s co-founder Josh Morrison calls them, “challengers”). And the roadblocks between where we are now, and implementing challenge studies, aren’t just logistical.
There are ethical questions, too. Is it okay to expose people to COVID-19? Under what circumstances? How can you make sure that they know the risks of the trial? What if they start the trial, and then they decide to leave before it ends? Are they willing to accept that participation in the trial might make them seriously and/or chronically ill? That they might die?
These are serious and complex ethical questions, but they’re not unique to challenge studies. All health care, and all medical research, involves ethically complex tradeoffs. Take surgery: a doctor cuts into someone, physically harming them, for the purpose of helping them get better. All research inconveniences participants to some degree, for the purpose of learning. Challenge studies exist on the same spectra—some harm, in hopeful exchange for some good—and scientists have been conducting challenge studies for hundreds of years.
But not challenge studies like this. “The field has gotten to a place where challenge studies are done in a fairly controlled fashion,” says Seema Shah, a bioethicist at Northwestern. Shah chaired a National Institutes of Health (NIH) ethics consult on challenge studies for the Zika virus. “The risks are minimized, and generally they’re done about diseases where either we know a lot about them, or there are treatments available, to prevent various complications.” We don’t know much about COVID-19 yet, and, as we all know too well, we don’t have many drugs to treat it. Under those conditions, challenge studies for COVID-19 would “take what’s accepted and move a step beyond that.”
But going a “step beyond” accepted medical study guidelines means facing incredibly complex, and interrelated, ethical tensions. Shah wishes people talked more about ethical “tradeoffs” in these studies. For instance, she says, “there are two issues that haven’t really been addressed in research ethics, and the two come into conflict” with challenge studies.
“In research ethics, we generally accept that people have the right to withdraw from research at any time without penalty. That is really important in challenge studies, because people have considerable burdens from participating in these studies, that they may not be able to anticipate in advance. But in a controlled human infection study, if you withdraw early, you might put third parties outside the research at risk. The question of exactly how to balance these two hasn’t been fully fleshed out.” If you want to leave the study early, you should be able to—but not at the cost of infecting other people. How can ethicists balance those conflicting principles?
Picture a Rube Goldberg machine, where a ball has to move through a hundred different mechanisms to trip a final switch. The machine’s broken, and it’s your job to fix it. Every time you adjust one of the mechanisms, another gets misaligned. Say you don’t want challenge study participants to get harmed by the trial, so you adjust the risk/benefit ratio in their favor by giving them money to participate. That money helps ensure that they’re benefiting from participation—but it increases the risk that people will sign up for the trial to earn money, and raises the possibility of coercion, potentially compromising the informed consent process.
Those interrelated complications would exist even in a well-resourced, and well-organized, country, and the US in 2020 is not that. It’s difficult to implement a risky study within a broken health care system. Take Shah’s example, of a study participant who decides to leave the study early: say, after exposure to the virus, but before they’re no longer contagious. “The public health authorities would put that person into quarantine,” she says, “but, as we know, public health authorities are very strapped at the moment, and they’re suffering a deficit of public trust.” Could researchers be certain that local public health authorities would ensure the safe at-home quarantine of participants leaving the study early?
There’s also the question of what would happen to “long-haulers”: people who get COVID-19 through a challenge study, and who suffer long-term health impacts. Shah says, “in the United States, we don’t have a guarantee that if you’re in a research study, you would get compensation for any injury that you suffered, especially for long-term injuries.” She contrasts the US with the UK, where research participants know that any long-term health effects of participation in a research study would be covered automatically, like all of their health care. Researchers in other countries are looking into COVID-19 vaccine challenge studies, including in the UK. Here in the US, Morrison and his colleagues have thought up some possible ways to pay for challengers’ long-term care, but those solutions are still hypothetical.
And there’s another major factor complicating the already tangled ethical web: the newness of COVID-19, and the speed with which what we know about the disease, and how well or poorly our response is going, changes. Back in April, Morrison co-wrote an opinion piece arguing for the necessity of challenge studies. He argued that social distancing would slow the spread of COVID-19, so much so that regular drug trials would take too long to yield results. If participants won’t get the virus, how can researchers test a vaccine? Now, Shah points out that just a few months have changed that situation. “The epidemic doesn’t seem to be that close to getting under control in the US,” she says. “There are just a handful of states who continue to seem to really have this under control. So I’m pretty skeptical that Phase 3 studies are going to fail because” the participants aren’t exposed to the virus.
Given this constantly-shifting, incredibly complex, incomprehensibly high-stakes situation, what’s a scientist to do? Nir Eyal co-wrote the paper that first got Morrison interested in challenge studies for COVID-19. Eyal argues for moving forward, although carefully. He mentions that “so far there are seven or eight peer-reviewed papers for [COVID-19 challenge studies], and none against,” which suggests agreement among most ethicists who have studied the issue. To the question of whether or not the studies will likely happen, he says, “it changes dramatically every two to three days, with our understanding of the virus.”
Shah offers a similar, but more tempered, take: “Challenge studies to address COVID-19 have a lot of potential, but shouldn’t be greenlighted right now. The risks are too uncertain, and the social value of these studies is also unclear. Until those two things change, it doesn’t seem right to go forward with them—but, in general, our group of diverse ethicists and challenge study researchers from around the world agreed that it would be a mistake not to prepare these studies, in case they are needed.”
Morrison characterizes his group, 1 Day Sooner, and Shah’s research coalition as mostly aligned. “Our actual public positions, when you boil them down, are not very different, [though] our tones are a bit different. I do think that I am much more likely to recommend a challenge study at the end of the day, or to have a more risky protocol than she would, but the position of her Science piece was, ‘there are no dealbreakers here, we should prepare,’ and our position is, ‘we’re optimistic this is useful and we’re not certain, and we should really prepare.'”
What does a more or less “risky” protocol actually mean? As Morrison, Eyal, and Shah all know, a participant might die, or might become seriously or chronically ill. That eventuality, Shah says, “could threaten the public perception of challenge studies in general, which are very important for other diseases, like malaria, for instance, and influenza.” A failed COVID-19 vaccine challenge study would likely also preclude the possibility of other such studies, even if conducted more cautiously. As Shah often writes, public trust in science, once lost, isn’t easily regained. It’s also worth noting that Morrison came to this issue in March, while Shah has been researching the ethics of challenge studies for years.
Shah says there’s a specific possible situation where she’d argue in favor of COVID-19 challenge studies: if we had one already-tested vaccine, and we wanted to compare it to a new one. “If we had a vaccine, and it was 50% effective—just past the barrier of what we think is enough—but it didn’t work well in some populations, or wasn’t as safe as we would like, or it was expensive and we needed more vaccines to bring down the cost. There could be lots of reasons to want to quickly compare other vaccines to the vaccine that’s been proven effective, and that, to me, could be a really important reason to do challenge studies.” Under such circumstances, Shah would support a challenge study; otherwise, otherwise, until the ethical and logistical conditions she’s listed are met, she thinks it’s too big a risk.
The same forces that inspire urgency in some people, like Morrison, inspire caution in others, like Shah. On the urgency side, getting a vaccine “one day sooner” could save lives, reopen the economy, allow kids to go to school, and so on. On the cautionary side, the conditions that make our world so in need of a vaccine make it more important than ever that we make no mistakes in developing one.
In other words, the choice facing researchers and would-be participants is a double-edged sword: erring on the side of caution with standard human trials could mean a longer wait for a vaccine, during which more people might die than would have otherwise. Challenge studies could shave time off vaccine development, but could hurt or kill participants, destroying public trust in research and public health. Potential catastrophes lie on both sides.