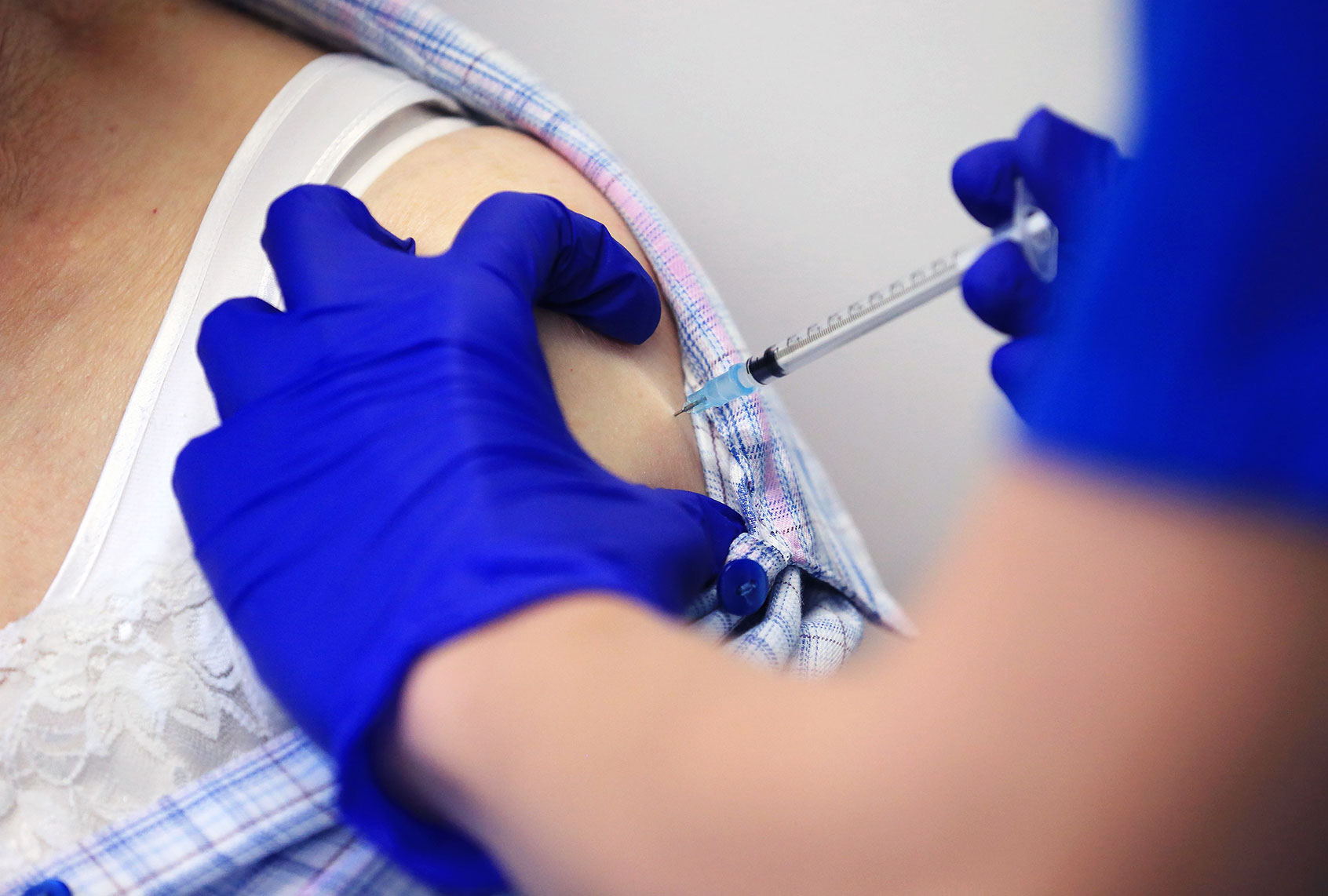
It’s been nearly six months since the first person in the U.S., nurse Sandra Lindsay, received the COVID-19 vaccine. Since patient one, over one hundred million Americans have been vaccinated. Indeed, as of Tuesday, at least 63.8 percent of U.S. adults have received one dose of the vaccine, according to the Centers for Disease Control and Prevention (CDC).
As vaccination rates increase, COVID-19 cases decline nationally, and the CDC continues to ease restrictions, more states and cities are fully re-opening. That means life in the United States is inching closer to “normal,” whatever that might mean post-pandemic.
Yet experts say that it is unclear if we are merely entering a brief respite, or if the pandemic is coming to its more permanent end. The reason? Researchers still don’t know how long immunity lasts for the vaccinated, and whether or not there will be a need for booster shots.
The idea that the coronavirus may require a booster shot is not new. Even at the pandemic’s dawn, it was a possibility, as it is relatively common for a vaccine to require a later booster; tetanus, diphtheria, and whooping cough are among the pathogens whose vaccines require later boosters.
A recent study of Pfizer’s SARS-CoV-2 vaccine found that it conferred an immunity that lasted at least 6 months. If immunity drops after a certain period, there may be a necessity for boosters.
Yet there are other factors that affect the need for booster shots besides the duration of immunity: mutations, too, will change the equation.
Amesh Adalja, a senior scholar at the Johns Hopkins Center, told Salon infectious disease experts are monitoring to see if fully vaccinated people get re-infected; and if so, how severe their cases are.
Want more health and science stories in your inbox? Subscribe to Salon’s weekly newsletter The Vulgar Scientist.
“To me, that’s the threshold you would use,” Adalja said. “So you would follow people that have been vaccinated, looking for breakthrough infections and see are more severe breakthrough infections occurring at a certain duration? That’s when you can kind of make that determination whether or not they’re needed.”
Dr. Charles Chiu, a professor of infectious diseases at the University of California–San Francisco, agreed with this threshold concept. Yet Chiu said that it’s too early to tell if we will need boosters at all, in part because not everyone in the U.S. is vaccinated.
“We will know that we need a booster when we start seeing an uptick in the number of infections in the vaccinated population, but right now it’s difficult to assess because we have significant portions of the population who are unvaccinated,” Chiu said. “If we get to, say, essentially herd immunity, we would know if need a booster by continuing to do surveillance of infection and monitoring for infections and [COVID-19] screenings.”
As Chiu alluded to, there is a debate over whether or not we will need booster shots at all. While Chiu said it’s perhaps “too early to tell,” he advised to be prepared for the possibility.
Besides boosters, seasonal vaccinations are a common practice among vaccines. Flu shots are offered once a year, and regularly updated to try to reflect the seasonal flu virus. Children who receive the MMR vaccine to protect against measles, mumps, and rubella, receive a first dose between 12 and 15 months of age and the second dose at 4 through 6 years of age. Not long ago, Salon interviewed infectious disease experts, Chiu included, who speculated that COVID-19 vaccines could be a seasonal shot.
Fortunately, the efficacy of the multiple COVID-19 vaccines have surprised many in the field and exceeded expectations. Yet immunity to COVID-19 doesn’t seem to last forever.
“We know that immunity elicited by the vaccines will wane over time, and the question is how fast is it going to wane. But eventually it probably will wane in such a way that we will need a booster,” Chiu added. He noted there was another looming reason that a booster might be necessary: mutations.
“The emergence of variants that can variably affect the effectiveness of the vaccine” may necessitate boosters, Chiu noted.
Adalja also said he believes it’s too early to say for sure.
“It’s especially premature . . . it takes time to study people who’ve been fully vaccinated to see if they get breakthrough infections,” Adalja said. “I don’t think it will be in the near-term based on what we’re seeing on this data for the general population, and that might be different for immunocompromised patients or people that are at high risk.”
But not all infectious disease experts agree. Monica Gandhi, infectious disease doctor and professor of medicine at the University of California–San Francisco, told Salon she doesn’t think we will need boosters for four main reasons. First, Gandhi pointed to one study that found that people with mild COVID-19 infections produce a “good T cell response,” meaning that the immune system’s memory is strong.
The immune system produces both B and T cells in response to an infection; B cells produce antibodies and T cells specifically attack and kill pathogens. Following vaccinations for other infections, like measles, mumps, rubella, pertussis, and diphtheria, T cell immunity is long lasting, as Gandhi explained.
Many scientists suspect that T cell immunity to SARS-CoV-2 will be just as durable (meaning long-lasting) as that of SARS 17 years ago. Gandhi pointed to a separate study on 12 people who were vaccinated with two Pfizer/BioNTech shots showing that the place where their memory B cells were stored in their lymph nodes increased in concentration over time — suggesting that even if antibodies fade, Memory B cells will linger for a while and be able to prevent against the original SARS-CoV-2.
But what about the variants?
“The antibody levels may be down against a specific variant, but your T cells that you produce from the vaccines produce multiple ‘epitopes’. . . and there’s about 100 T cells that line up across the spike protein to help you fight the infection after vaccination,” Gandhi said.
“And so even if you have a variant that has 13 mutations, like the Delta variant which a lot of mutations, you’re still going to get that lineup of lots of T cells that combat some of those variants. So I do think T cell responses from vaccines will work against them.”
Hopefully, new variants will be a moot issue. Chiu said it could be possible to stop new variants from emerging, but that possibility hinges on the entire world being vaccinated.
“One thing that has to be kept in mind is that still the rest of the world is largely not immune, and the rest of the world has not really been vaccinated,” Chiu said. “The reason why these variants emerge is because you have ongoing transmission, so until we’re able to curtail the pandemic globally, we’re going to continue to see the emergence of variants.”
Chiu emphasized this is a major concern, as it could influence the need for booster shots.
Notably, in some countries, booster shots are already being administered. According to AP News, the United Arab Emirates is offering boosters to people who received the Sinopharm vaccine. Adalja said that doesn’t necessarily foreshadow what will happen in the United States.
“The Sinopharm has not published phase three clinical data, so we don’t have a good strong understanding of how efficacious it is,” Adalja said. “But what we do know is that both the Sinovac and Sinopharm seem to not work as well as Moderna, Pfizer, AstraZeneca, Johnson & Johnson — so there may be some specific issues with that vaccine.”